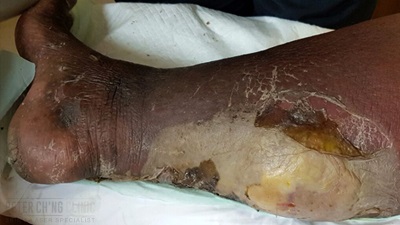
Treatment for Ringworm

What may put me at higher risk getting infected by ringworm?
First of all, ringworm is not due to worm infestation. It is actually a layman term for fungal infection of the skin, hair or nails. Fungus loves warm and moist areas. Therefore it is common to see ringworm infection in humid countries such as Malaysia. If you have direct (skin to skin or skin to surface that contains fungus) contact with active lesion of an infected patient or pet, you may also be at higher risk of getting infected by ringworm. You will also be at higher risk of getting ringworm infection if you have a weakened immune system such as Diabetes Mellitus, HIV and cancer.
Are there complications related to ringworm?
Ringworm of the scalp can cause permanent hair loss. Ringworm may also cause itchiness and if the patient scratches the skin lesion, there is always risk of secondary bacteria infection and scarring. Ringworm of the nails can also cause discoloured or destroyed nails.
How can I prevent from ringworm at the first place?
Avoid sharing towels and clothing. Try to avoid barefoot in wet common areas such as swimming pool and bathroom. Keep your skin clean and dry. Change your socks and underwear daily. If you sweat, rest for half an hour before bathing. Do make sure that your skin folds are dry especially over the groin and toe web spaces. Whenever possible, avoid tight clothing. If you have a pet with suspected skin disease such as loss of hair, bring to a veterinarian.
What is the treatment for ringworm infection?
Treatment depends on the site and extends of the infection. If it involves hair or nails, or the skin infection is extensive, oral antifungal such as griseofulvin, imidazoles or allylamines group of antifungal is required.
For localized or when small area of the skin is involved, topical antifungal treatment is sufficient. Topical antifungals treatments that are widely available in Malaysia are:
Imidazole
- Miconazole
- Sertaconazole
- Clotrimazole
- Ketoconazole
Allylamines
- Terbinafine
Substituted pyridines
- Ciclopirox
Topical antifungals should be applied 2 cm beyond the margin of the rash and continue to apply for another 2 weeks after the symptoms resolved. Mild to moderate potency topical steroid is sometimes used for short term to reduce down the inflammation and itchiness but should be used cautiously. If topical steroid is used alone, it can actually worsen the fungal infection. Besides treating the infection, identifying the source of fungal infection is also important to prevent relapse. For example, a fishmonger who wears boots all the time is going to have a relapse if there is no modification to his job. As for patients with Diabetes Mellitus, good sugar control is important to prevent relapse.
What is pityriasis versicolor?
Pytriasis or Tinea versicolor is also known as “ Panau” among the locals. It presents as scaly white, dark or pink rash over the trunk or arms. A type of fungus (yeast) that normally lives harmlessly on our skin causes this condition. Under certain condition such as warm, humid environments, weakened immune system and malnutrition, this yeast will proliferate and caused problem to our skin. Pytriasis versicolor is not contagious although some patients may say that there are family members who are having similar condition. This is because some of the patients have genetic predisposition to this condition.
What is the best way to treat pityriasis versicolor?
Patients should be informed that this condition is not contagious or dangerous. Even with effective treatment, the difference in colour will only turn to normal after weeks or even months.
For mild cases, patient can apply cream, ointment, lotion or shampoo such as:
- Miconazole
- Ketoconazole shampoo
- Selenium sulphide shampoo
- Clotrimazole
- Ciclopirox
- Sodium thiosulphate solution
Proper application of the topical medication is important for it to be effective. For cream, ointment or lotion apply twice daily on the affected skin for at least 2 weeks. For shampoo, leave it on the affected skin for at least 10 minutes before rinsing off. Shampoo can be used twice a month to prevent recurrence.
How to get rid of persistent pityriasis versicolor?
For persistent pytriasis versicolor, oral itraconazole or fluconazole can be used if there is no contraindication and the risk versus benefit of oral antifungal has been explained to the patient.
To enquire more about Treatment for Ringworm, contact us or book an appointment here!
This treatment can treat the following conditions:
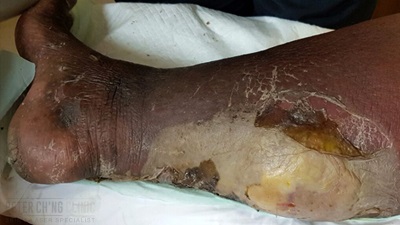
Skin Diseases and Cancers
Skin infection ranges from bacteria, fungus, virus to parasite. Skin cancer is more accurately differentiated from benign tumour using a dermatoscope. If the tumour looks suspicious, skin biopsy or complete excision of the tumour can be done.
Related treatments and services:
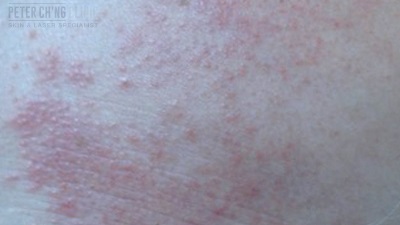
Treatment for Eczema
Atopic eczema or atopic dermatitis is the commonest skin condition in children. Almost 1 in 5 of the children in Malaysia are suffering from atopic eczema.
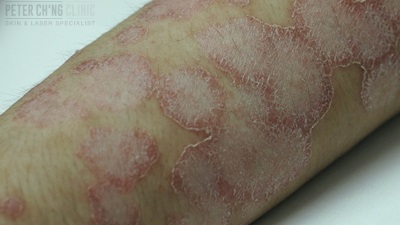
Treatment for Psoriasis
People with psoriasis know that this condition is no mere skin disease. Their skin forms red patches with thick, silvery scales, and these plaques are accompanied by itch, irritation and even joint pain.